Oral Cancer- Tips to Improve your Oral Examination
- Amanda Phoon Nguyen

- Feb 4, 2022
- 4 min read
For World Cancer Day 2022: Closing the Gap
Worldwide, oral cancer is a significant health burden and is recognized as the sixth most common cancer. In Australia, oral cancer accounts for about 2-3 per cent of all cancers. A trend in decline of the incidence of lip and oral cavity cancer, and a rise in the incidence of oropharyngeal cancer has been reported. However, survival rates have not dramatically improved in the last few decades, despite advances in treatment and management options. Overall survival rates for oral cancer are poor, at about 50 per cent for all anatomical sites and stages. When looking at studies, the use of the term “oral cancer” can sometimes be confusing. Oral cancers are a heterogenous group of conditions encompassing the main subsites of the external lip, oral cavity and oropharynx, and it is important to consider this when reading articles which specific subsite the paper refers to, as the aetiology, management and prognosis of lip cancer, oral cavity cancer and oropharyngeal cancer differs.
Tips
Early detection of potentially malignant disease has been proven to improve the clinical outcome for patients, and therefore it is very important to perform thorough intra and extraoral examinations for every patient. How could we improve the patient risk evaluation and conventional visual screening of oral tissues?
1. Taking a good history
It is important to take a good history and note any factors which may put the patient at a higher risk of oral cancer. This may include current or a history of smoking, alcohol consumption, smokeless tobacco use, use of an alcohol containing mouthwash, and a family or personal history of cancer.
2. Awareness of the suspicious changes
Changes to the oral mucosa are detected visually due to light interaction with tissue. As the tissue changes, there are colour alterations which we can see. The most common are white and red changes to the mucosa. Changes can appear as an ulcerative, flat, raised or exophytic, red and/or white lesions. The oral cavity can also be the site of cancer metastasis from other parts of the body, most commonly of breast, kidney and lung. Signs such as firmness to palpation, pain and ulceration are more commonly seen when the lesion is already malignant. The poor prognosis of oral cancer can largely be attributed to its frequent diagnosis at an advanced stage, and early detection is key. Early lesions are usually asymptomatic.
3. Using the appropriate lighting
The use of loupes and/or a LED headlight, where available, will assist with the examination. Examination with the naked eye should be under white light where possible (projected incandescent or halogen illumination).
Actinic cheilitis, also termed actinic cheilosis, actinic keratosis of the lip, solar cheilosis, sailor’s lip, and farmer’s lip, is a type of lip inflammation caused by long-term sunlight exposure. The prolonged solar exposure produces irreversible damage to the lower lip, and this is very common in Australia. It is a premalignant condition that could develop into squamous cell carcinoma. Signs include the loss definition of the vermilion border and mucosal changes to the lips, such as dry or mottled skin, white or grey plaques or patches, and crusting. Persistent ulceration, crusting or firmness to palpation should be viewed with suspicion.
4. Check the tissues in a systematic manner
The development of a consistent examination sequence is important. While the order of this does not matter, all elements must be completed. Before looking in the mouth, a thorough extraoral examination should not be missed. This should include a general examination of the patient and inspection of the temporomandibular joints, facial skin, lymph nodes, neck, midline neck structures, lip and perioral structures. By doing the same sequence for all patients, clinicians are more likely to consistently check all sites.
High risk sites for oral cavity squamous cell carcinoma includes the lateral and ventral tongue, and floor of mouth. Other areas which are frequently missed include the soft palate, posterior lateral tongue and oropharynx.
5. Palpate as well as visually inspect structures
Besides looking at structures, it is also important to palpate them. Two worrying signs are induration and fixation. Induration is where there is an increase in the tissue density (the tissue becomes hard), and fixation is loss of tissue mobility, where the tissue does not move. Cancer can cause tissues to become indurated and fixed.
6. Refer or review
Most oral mucosal lesions of traumatic aetiology will resolve within 2 weeks, once the cause is removed. A common scenario is a chipped tooth causing tissue changes (such as a white patch) of the adjacent mucosa. The tissue should return to a normal appearance once the tooth is smoothed, and this should be ascertained with a review after 2 weeks. Good recall systems should be in place to ensure the patient returns for the review and the appointment is not missed. Any oral mucosal lesion which persists beyond 2 weeks should be viewed with a degree of suspicion. This patient should be referred directly to the appropriate specialist, such as an oral medicine specialist.
Figure 1: Tissue changes involving the floor of mouth

Figure 1: Tissue changes involving the floor of mouth

Figure 2: Tissue changes involving the right buccal mucosa and lateral tongue
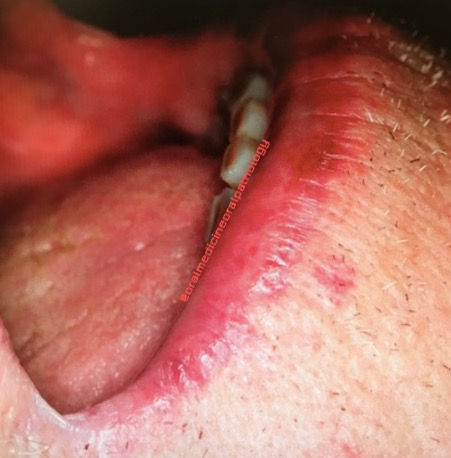
Figure 3: Loss of definition of the vermilion border and crusting involving lower lip
Figure 3: Loss of definition of the vermilion border and crusting involving lower lip


Comments